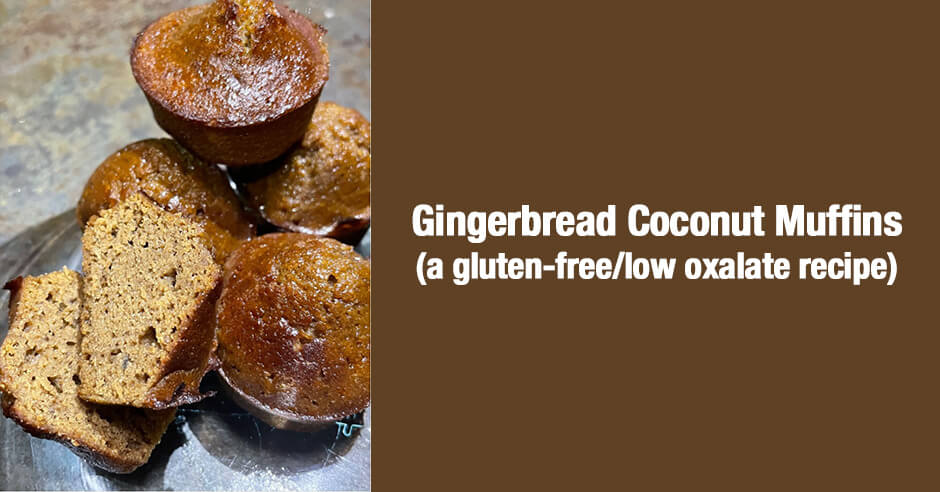
If you have gluten sensitivity or celiac disease and/or dietary oxalate issues (pain, anxiety, insomnia, restless legs, hearing loss, eye issues, unresolved thyroid issues, bladder issues and more) and yet really miss the occasional muffin this Gingerbread Coconut Muffins recipe is a delicious gluten-free and low oxalate option. I see way too many so-called healthy gluten-free recipes using almond flour. This is concerning given that almonds are high in oxalates. Keep in mind that wheat is also high oxalate.
I’m finding dietary oxalate issues to be underappreciated especially in menopausal women when symptoms can show up and be more severe. If you’re new to the dietary oxalate issues you can read more below.
I have also found that using almond flour and other nut flours in baking affects your zinc/copper balance, increasing copper and hence causing more anxiety and even panic attacks.
If you don’t have dietary oxalate issues, you can certainly enjoy this recipe too. But watch the overindulging and binge-eating (more on that and using amino acids below).
Gingerbread Coconut Muffins (a low oxalate recipe)
Ingredients
6 eggs
1/3 cup melted butter
1/4 teaspoon salt
1/2 cup molasses
1/2 cup coconut sugar
2-3 teaspoons ginger powder (or liquid ginger extract)
3/4 cup sifted coconut flour
1 tablespoon ground flax seeds
Method
Melt the butter over low heat and add the coconut sugar and molasses. Once it’s cooled add the eggs and mix well. Stir in the coconut flour, salt, ground flax seeds and ginger powder.
Spoon the mixture into two greased mini muffin pans. Bake at 400 degrees F/ 205 degrees C for 12 – 14 minutes. The muffins will rise nicely and will start to turn dark brown. Remove and cool on a cooking rack. Makes 24 mini muffins.
Eat warm or when cooled. Serve with butter and/or cream and/or coconut butter. For a little added sweetness a small amount of raw honey can be spread on a muffin too.
My adaptation from a gingerbread cookies recipe
I adapted this recipe from a Gingerbread Cookies recipe in Cooking with Coconut Flour by Bruce Fife ND. I pretty much always do this when I cook – adapt recipes to my needs and likes – and always reduce the sugar. In this instance, I halved the sugar and used coconut sugar instead.
I also increased the ginger because I love all things ginger. I upped it from 1 teaspoon ground ginger to 2 teaspoons and will actually try 3 teaspoons next time I make them. Ginger can be an issue if you have oxalate issues so you’d want to see how much you can tolerate – so far so good for me. If you do have issues with ground ginger you could always use a liquid ginger extract which is low oxalate.
I omitted the cinnamon and cloves to emphasize the ginger taste. I also added ground flax seeds for added fiber.
I decided to cook them in mini muffin pans instead of making cookies on a baking tray but you could always try this option. Use the same temperature and cooking time per the original recipe.
The blackstrap molasses makes them so flavorful too and takes me back to my childhood. Molasses is nutrient dense too, providing calcium, magnesium, potassium, manganese, iron, vitamin B6, and selenium. Just be sure to use molasses made from sugar cane and not sugar beets (which are high in oxalates).
They were surprisingly soft and moist and eating them with butter and/or cream made them even more delicious. I always like to include some healthy fats. If dairy isn’t tolerated, coconut cream could be substituted. I suspect coconut oil could be substituted for the melted butter but have not tried this yet.
Here is Cooking with Coconut Flour by Bruce Fife ND. You can find it on Amazon here (my link). I’ve baked a number of recipes from this book and I’m impressed. I really appreciate that it’s all coconut flour recipes with no almond flour or other gluten-free flours used.
If you do battle with sugar cravings and binge eating – use amino acids
It’s ideal to keep baked goods – especially the ones shown on the cover of this book – to a minimum. But for an occasional treat this recipe book is excellent.
If you do battle with sugar cravings and binge eating, don’t forget how useful the amino acids are for stopping your cravings with no willpower and no feelings of deprivation. You can learn more about this here: The individual amino acids glutamine, GABA, tryptophan (or 5-HTP), DPA and tyrosine are powerful for eliminating sugar cravings, often within 5 minutes.
I discuss cravings/emotional eating and how to use amino acids in my book, The Antianxiety Food Solution – How the Foods You Eat Can Help You Calm Your Anxious Mind, Improve Your Mood and End Cravings. More here. I also cover how low blood sugar can lead to both anxiety and cravings and how to prevent this by use glutamine and eating for blood sugar stability.
If you’re new to dietary oxalates as a possible health issue
This blog post is a helpful one to start with if you’re new to dietary oxalates and the issues they can cause: Oxalate crystal disease, dietary oxalates and pain: the research & questions
These are the common medium-oxalate and high-oxalate foods that many folks have problems with: nuts, nut-butters and nut-flour (especially baking with almond flour and something to watch when eating Paleo or GAPS), wheat, chocolate, kiwi fruit (very high – see the raphides image on the above blog), star fruit (also very high), beets, potatoes, sweet potatoes, legumes, raspberries, spinach and soy.
In the above blog post, I share an overview of oxalates, my pain issues with dietary oxalates (severe foot pain and eye pain), and deeper dive into the condition called oxalate crystal disease (with some of my insights and questions).
The big take-aways are that calcium oxalate crystals are sharp and can cause far reaching harm beyond pain – such as unresolved anxiety, thyroid issues, neurological symptoms, eye issues, hearing loss, bladder issues, headaches, fatigue, insomnia, restless legs, autism symptoms and more. You can have issues with dietary oxalates and not have kidney disease/kidney stones, although there is very little research supporting the latter.
You may find these oxalate blogs helpful too:
- Increased kidney stones in postmenopausal women with lower estradiol levels. What about increased dietary oxalate issues too?
- Waking in the night due to environmental toxins: impacts on the liver, gallbladder and fat digestion (making oxalate issues worse)
- Butternut Bake recipe (a low oxalate alternative to Potato Bake)
- Coconut Macaroon Mini Muffin recipe (low oxalate)
What dietary oxalates issues have you experienced and has a low oxalate diet helped you?
If you have dietary oxalates issues can you handle ginger?
Do let us know if you make this recipe and enjoy it.
Feel free to share a favorite recipe of something you’ve adapted to be low or even medium oxalate.
If you have questions and feedback please share them here too.







