Today I’m sharing some highlights from a recent eye-opening article in the Washington Post: A catatonic woman awakened after 20 years. Her story may change psychiatry
Before she became a patient, April had been an outgoing, straight-A student majoring in accounting at the University of Maryland Eastern Shore. But after a traumatic event when she was 21, April suddenly developed psychosis and became lost in a constant state of visual and auditory hallucinations. The former high school valedictorian could no longer communicate, bathe or take care of herself.
April was diagnosed with a severe form of schizophrenia
April was hospitalized, medicated and eventually institutionalized. It got to the point where she no longer recognized her family and she became catatonic, “unmoving, unblinking and unknowing of where or who she was.”
Twenty years after April’s original diagnosis it was discovered that she has an autoimmune condition. Dr. Sander Markx is director of precision psychiatry at Columbia University and I have so much admiration for his dedication to the field and the fact that he facilitated this testing and discovery so long after meeting April, when he was a student:
Markx and his colleagues discovered that although April’s illness was clinically indistinguishable from schizophrenia, she also had lupus, an underlying and treatable autoimmune condition that was attacking her brain.
After months of targeted treatments – and more than two decades trapped in her mind – April woke up.
April’s transformation is truly heartwarming and it’s wonderful that the doctors plan to do similar testing and offer similar treatments for others living with schizophrenia who are in mental health institutions in New York State.
Researchers in other countries are making similar connections and it’s really exciting to read that they are recognizing that “underlying autoimmune and inflammatory processes may be more common in patients with a variety of psychiatric syndromes than previously believed.”
We can and should be doing better when looking for root causes
I believe we can and should be doing better when it comes to looking for root causes. Many individuals may have an autoimmune/inflammatory condition and many may have other root cause/s. If I was on an advisory panel these would be my recommendations:
- Use this powerful outcome to really turn psychiatry on its head and screen for lupus and other autoimmune conditions in every single person with schizophrenia. Dr. Markx “believes highly sensitive and inexpensive blood tests to detect different antibodies should become part of the standard screening protocol for psychosis.”
- Do the same for every single person with mental illnesses and illnesses with a behavioral aspect – including anxiety, depression, bipolar, OCD/obsessive compulsive disorder. ADD/ADHD, autism/ASD (autism spectrum disorders), developmental disorders and neurological disorders.
- Go beyond autoimmune screening and do a comprehensive functional medicine and nutritional deficiency assessment for every single person, including low serotonin, low GABA, low vitamin D, low zinc, low vitamin B6, hormone imbalances (sex hormones, adrenals, thyroid health), gut health, liver health etc. This includes testing for infections (such as Lyme and strep), looking at toxin exposure (phthalates, mold, heavy metals) and medication side effects.
If you’re new to the concept of root causes and functional medicine/nutritional testing these two blogs will be helpful. They are specific to anxiety because I work with anxious individuals but much of it can also be applied to other mental health and even physical health conditions (like rheumatoid arthritis and say multiple sclerosis):
- Nutritional testing for figuring out the root cause/s of your anxiety
- 60+ Nutritional & Biochemical Causes of Anxiety
Functional medicine and nutrition for maintaining symptom resolution in the long term
As you read in the article, April received “short, but powerful “pulses” of intravenous steroids for five days, plus a single dose of cyclophosphamide, a heavy-duty immunosuppressive drug typically used in chemotherapy and borrowed from the field of oncology. She was also treated with rituximab, a drug initially developed for lymphoma.”
Incredibly, she recovered completely and was eventually discharged from the psychiatric hospital and has been living in a rehab center for 3 years. Unfortunately “she has recently regressed because she was not receiving adequate maintenance care.”
I see the next step for April and others like her, is maintaining resolution of symptoms in the long term. This is where functional medicine and nutrition shines.
The ISNPR shared this about Nutritional psychiatry in 2015 in a letter published in World Psychiatry, the official journal of the World Psychiatric Association:
In addition to dietary modification, we recognize that nutrient-based (nutraceutical) prescription has the potential to assist in the management of mental disorders at the individual and population level.
In other words, diet and nutrient-based approaches need to be included for mental health treatment and for prevention. One of many examples is the ketogenic diet which has been shown to reduce auditory hallucinations and delusions in those with schizophrenia. Another is the low carb diet helping to reduce bizarre intrusive thoughts. And the SMILES trial was the first randomized controlled trial to show that dietary improvement can actually treat depression.
Specific nutrients can be very powerful too. One example is a case where a woman in my community experienced a drastic reduction in intrusive thoughts, anxiety and fears (and better sleep) with GABA, tryptophan, 5-HTP and the pyroluria protocol (zinc, vitamin B6 and evening primrose oil). More on the blog. Intrusive thoughts can be alleviated with a similar combination of nutrients and by addressing hormonal imbalances too.
These blogs/research illustrate a few of the many root causes of schizophrenia and psychosis other than lupus:
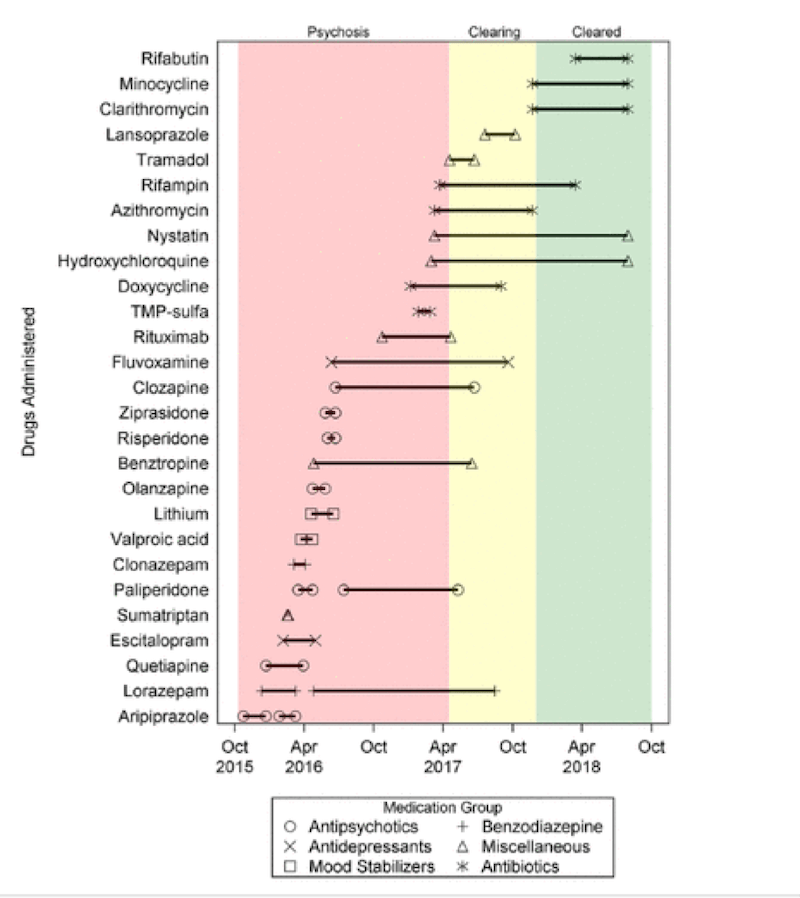
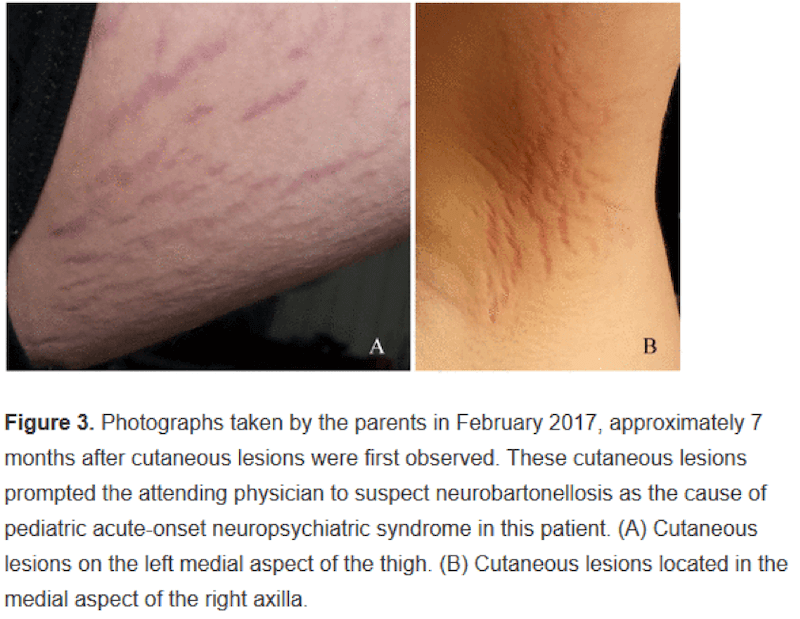
- Case Study: Bartonella and Sudden-Onset Adolescent Schizophrenia
- Toxoplasma gondii: schizophrenia, bipolar disorder, OCD and unresolved anxiety?
-
Gluten sensitivity and relationship to psychiatric symptoms in people with schizophrenia
When it comes to autoimmunity in general I refer you to the work of Dr. Tom O’Bryan, Dr. Izabella Wentz, Dr. Terry Wahls, Dr. Amy Myers and others who teach about using functional medicine and diet for reversing a number of different autoimmune conditions.
The above approaches can all be explored and used when individuals are initially diagnosed too. But keep in mind that there is no one size fits all and it’s a matter of finding the root causes for each person.
We are moving in the right direction and there is hope but…
We are moving in this direction, awareness is growing and there is hope. But I know we can get there sooner.
What Dr. Markx and his colleagues have discovered and shared with the world will hopefully help us get there much more quickly.
(You can read the whole story here and a similar transformation experienced by Devine Cruz.)
I’m thrilled for April and Devine and their families, and appreciate them sharing these stories with the world. Let’s hope their stories do change psychiatry!
Resources if you are new to using amino acids as supplements
If you are new to using amino acids as supplements, here is the Amino Acids Mood Questionnaire from The Antianxiety Food Solution (you can see all the symptoms of neurotransmitter imbalances, including low GABA, low serotonin and low endorphins).
If you suspect low levels of any of the neurotransmitters and do not yet have my book, The Antianxiety Food Solution – How the Foods You Eat Can Help You Calm Your Anxious Mind, Improve Your Mood, and End Cravings, I highly recommend getting it and reading it before jumping in and using amino acids on your own so you are knowledgeable. And be sure to share it with the practitioner/health team you or your loved one is working with.
There is an entire chapter on the amino acids and they are discussed throughout the book in the sections on gut health, gluten, blood sugar control, sugar cravings, anxiety and mood issues.
The book doesn’t include product names (per the publisher’s request) so this blog, The Antianxiety Food Solution Amino Acid and Pyroluria Supplements, lists the amino acids that I use with my individual clients and those in my group programs. You can find them all in my online store.
If, after reading this blog and my book, you don’t feel comfortable figuring things out on your own (i.e. doing the symptoms questionnaire and respective amino acids trials), a good place to get help is the GABA QuickStart Program (if you have low GABA symptoms too). This is a paid online/virtual group program where you get my guidance and community support.
If you are a practitioner, join us in The Balancing Neurotransmitters: the Fundamentals program. This is also a paid online/virtual program with an opportunity to interact with me and other practitioners who are also using the amino acids.
Does this heartwarming story give you hope for psychiatry?
What do you feel we should be doing to advance nutritional psychiatry even more quickly?
Can you or a family member relate to this and what did you discover in terms of testing and nutritional support/functional medicine?
Feel free to post your feedback and questions here in the comments.